By The AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE Formerly The American Fertility Society
What is a hysterosalpingogram (HSG)?
An HSG is an x-ray procedure performed to determine whether the fallopian tubes are open and to see if the shape of the uterine cavity is normal. An HSG is an outpatient procedure that takes less than half an hour to perform. It is usually done after menstruation has ended, but before ovulation, to prevent interference with an early pregnancy.
How is an HSG done?
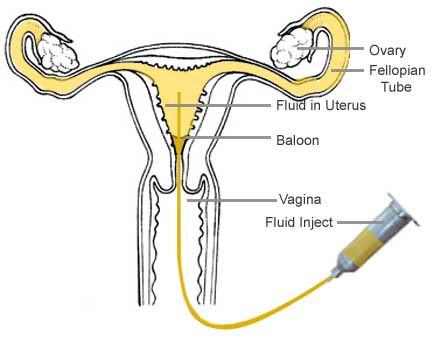
A patient lays on a table under a fluoroscope (a real-time x-ray imager). The gynecologist or radiologist then does a pelvic exami-nation, places a speculum in the vagina, cleans the cervix, and places a device (acorn cannula) into the opening of the cervix. The physician then gently fills the uterus with a liquid containing iodine (contrast) through the cannula. The contrast then enters the tubes, outlines the length of the tubes, and spills out their ends if they are open. Any abnormalities in the uterine cavity or fallopian tubes will be visible on a monitor. The HSG is not designed to evaluate the ovaries or diagnose endometriosis. Frequently, side views of the uterus and tubes are obtained by having the pa ‘znt change her position on the table. After the HSG, a patient can immediately resume nor-mal activities, although some physicians ask that the patient refrain from intercourse for a few days.
Is an HSG uncomfortable?
An HSG usually causes mild or moderate uter-ine cramping for about five minutes; however, some women may experience cramps for several hours. The symptoms can be greatly reduced by taking medications used for menstrual cramps.
Does a hysterosalpingogram enhance fertility?
It is controversial whether this procedure enhances fertility. Some studies indicate a slight increase in fertility lasting about three months after a normal HSG. Most physicians perform the HSG only for diagnostic reasons.
What are the risks and complications of HSG? An HSG is considered a very safe procedure. However, there are some rec-ognized complications, some serious, which occur less than 1% of the time.
• Infection — The most common serious problem with HSG is pelvic infection. This usually occurs in the presence of previ-ous tubal disease. In rare cases, infection can damage the fallopian tubes or necessitate their removal. A woman should call her doctor if she experiences increasing pain or a fever within one to two days of the HSG.
• Fainting — Rarely, the patient may get light-headed during, or shortly after, the procedure.
• Radiation Exposure — Radiation exposure from an HSG is very low, less than from a kidney or bowel study. There have been no demonstrated ill effects from this radiation, even if conception occurs later the same month. The HSG should not be done if pregnancy is suspected.
• Iodine Allergy — Rarely, a patient may have an allergy to the iodine contrast used in an HSG. A patient should inform her doctor if she is allergic to iodine or seafood. Non-iodine contrasts are available for allergic patients. If a patient experi-ences a rash, itching, or swelling after the procedure, she should contact her doctor.
• Spotting — Spotting commonly occurs for one to two days after the HSG. A patient should notify her doctor if she experi-ences heavy bleeding after the HSG.



Add a Comment