Key Facts about cervical cancer in Malaysia
- Cervical cancer is the 2nd most common cancer affecting Malaysian women, after breast cancer
- In 2002, cervical cancer accounted for 12.9% of all female cancer in Malaysia
- Virtually every woman is at risk of cervical cancer, regardless of their age or lifestyle.
- Current estimates in 2017 indicate that every year 2145 women are diagnosed with cervical cancer and 621 dies from the disease.
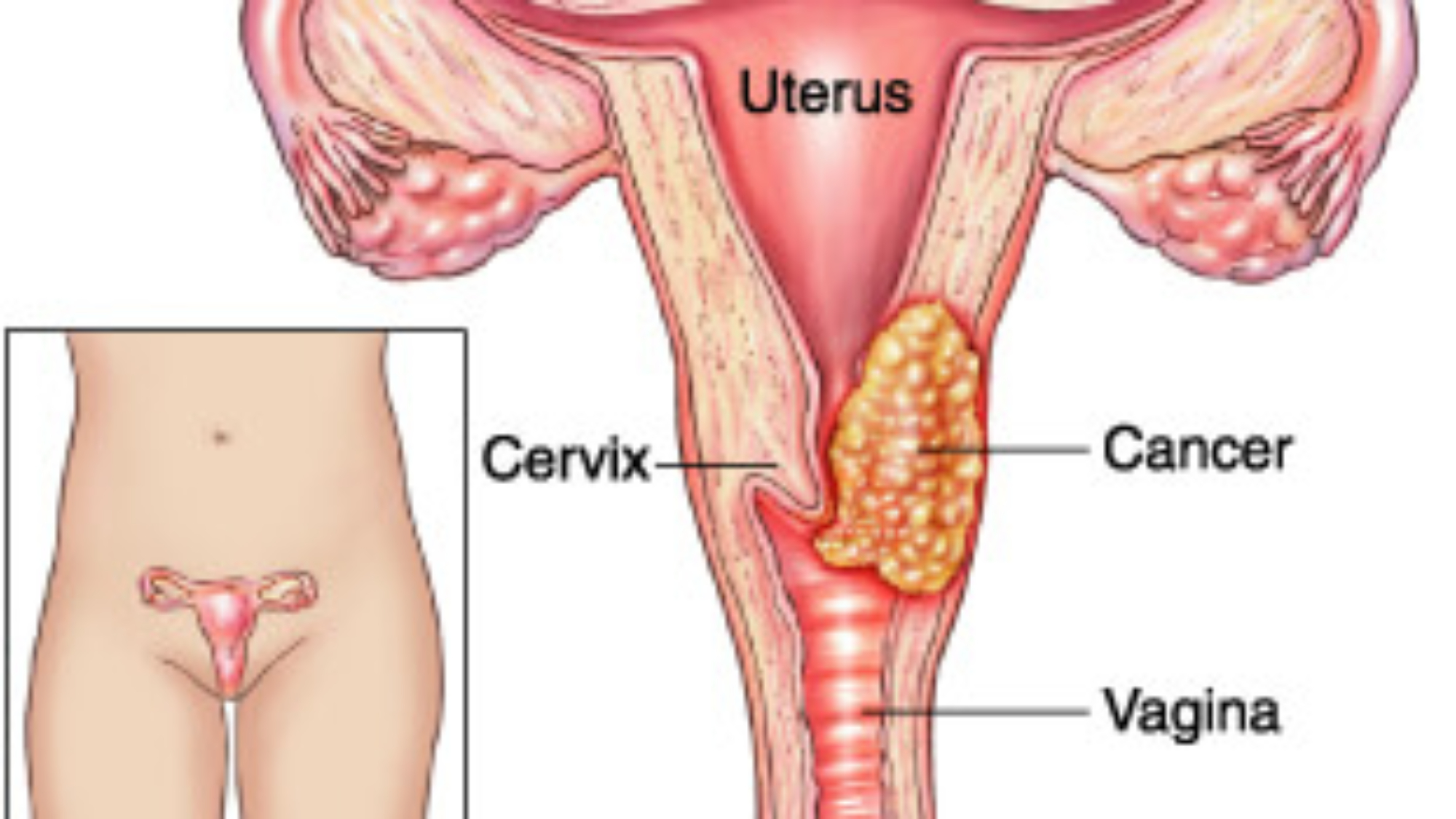
Q: What Is Cervical Cancer?
A: The cervix is the neck of the womb (uterus). It connects the body of the uterus to the vagina (birth canal). Cancer occurs when the cells of the cervix become abnormal and grow out of control. Cancer can spread to other parts of the body.
Q: What is HPV (human papillomavirus)?
A: Human papillomavirus (HPV) is a family of more than 100 viruses that is very common. Some types of HPV are associated with certain types of cancer. These are called “high-risk” cancer-causing HPVs.
Q: What is the relation between HPV and Cervical Cancer?
A: Most HPV infections occur without any symptoms and will go away without any treatment over the course of a few months.
Infection by the “high risk” (cancer-causing) HPV is necessary for the development of cervical cancer. These infections are asymptomatic and the majority will resolve without any need for treatment. However, in some cases, the infection can persist, leading to the risk of progression to cervical cancer. This process can take more than ten years. Therefore it is important to be protected against the “high-risk” (cancer-causing) HPVs.
Q: How is HPV transmitted?
A: HPV is a common virus that is transmitted through genital skin to skin contact so it can affect virtually any woman, regardless of her age or lifestyle. Sexual intercourse is not necessary to become infected. It is estimated that about four out of five sexually active women will have an HPV infection during their lifetime, even if they’ve only had one or two sexual partners.
Q: Will I still be at risk of HPV infection if I am already married?
A: The risk of HPV infection starts from the first sexual encounter and lasts throughout a woman’s life. It is estimated that up to 80% of women will acquire a genital HPV infection in their lifetime irrespective of their age or lifestyle.
Q: Do condoms reduce the risk of HPV infection?
A: Condoms reduce the risk but are not fully protective. Throughout her life, every woman is at risk from the virus that causes cervical cancer.
WHAT CAN BE DONE?
This is the best way to reduce your risk of cervical cancer is to have a pap smear done. Regular Pap tests can prevent around 90% of cervical cancers.
Q: What is a Pap smear?
A: A Pap smear is a quick and simple test to find abnormal cells at the surface of the cervix. Usually, cells are collected from the cervix and sent to a laboratory where they are tested for changes.
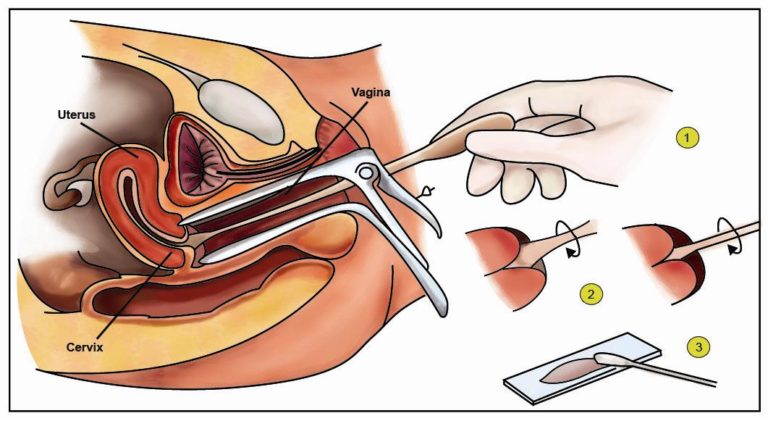
Q: Who should get a pap smear?
A: All women aged 18 to 70 who’ve ever been sexually active should have a Pap test every 2 years, even if they’re no longer having sex.
Q: Can Cervical Cancer be prevented?
A: Until recently the only way to prevent cervical cancer was regular Pap smear testing to look for early signs of the disease. Vaccination is now available to prevent HPV infection and cervical cancer.
Talk to your Doctor about protecting yourself and your loved ones.
LIQUID-BASED CYTOLOGY (LBC)
Cervical cancer is a highly preventable disease. Undergoing regular pap smear is the most important means of prevention’. However, the pap smear has a significant false-negative rate of up to 20% which mainly happens during the slide preparation. There is also the issue of unsatisfactory tests due to inadequate sampling and preparation resulting in tests having to be repeated. Newer techniques are now available.
What is Liquid-Based Cytology (LBC)?
Liquid-Based Cytology (LBC) is a new cervical cell collection technique developed from the conventional method, the pap smear. It aims to address some of the limitations of the pap smear and enhance the detection of pre-cancerous lesions by improving sample collection and cell preparation. Unlike pap smear where the cervical cells are smeared directly onto the glass slide by the clinician, with LBC, cervical cells sample is placed in a vial of preservative and sent to the laboratory where the final slide is produced.
Why perform the test?
For the screening and detection of cervical cancer, pre-cancerous lesions, atypical cells and other cytological categories.
Why Use LBC?
- More likely to produce a good set of cells for microscope reading
- Lowers the rate of unsatisfactory tests, reducing women’s anxiety and need for repeat smears
- Red blood cells, inflammatory cells, mucous and other interfering substances removed, enabling clean observation of cells and reduces the number of unsatisfactory tests.
- Has the potential to detect more pre-cancerous lesions.
- Has the potential for multiple slide preparation from the same cell suspension and to allow additional testing from a single vial (eg. HPV DNA Genotype).
- Air-drying artifact, the cause in many limited or inadequate pap smears, non-existent due to the transfer of cells directly into a liquid medium at the time of collection.
HPV DNA Genotype
What is it?
There are many types of Human Papillomavirus (HPV). Low-risk HPV types are associated with genital and other skin-related warts whereas high-risk types are associated with cervical cancer. Persistent infection with a high-risk type is the major cause of cervical cancer.
What is HPV DNA Genotype?
HPV testing is available to detect HPV DNA in cervical cells and determine the strain of Human Papillomavirus (HPV). The test can be performed on the residual cells of an LBC sample. This test can detect 15 high risk HPV strains: 16, 18, 31, 33, 35, 39, 45, 51, 52, 53, 56, 58, 59, 66, 68 and 5 low-risk strains : 6, 11, 41, 42, 44, which are responsible for 99.7% of genital warts.
Why perform the test?
- Enhanced screening for cervical cancer
- Earlier detection. The presence of virus can be detected before cell changes in the cervix have occurred.
- If tested positive for HPV but LBC indicates no abnormal cell changes, condition can be closely monitored and decision can be made on what follow-up is necessary
Combination
With the combination of both Liquid-Based Cytology a DNA Genotype test, the detection of cervical cancer can be greatly improved.
Annual screening of HPV testing paired with LBC is more cost saving and effective.
- The combination of both tests can reduce colposcopy referrals, an incidence of cervical cancer and related mortality.
- HPV testing and LBC screening combined can reduce disease incidence at a 2-year screening interval.
- HPV testing can be performed on residual cells of an LBC sample. Does not require the collection of a second sample.
- A decrease in the number of deaths would ultimately result if lesions were detected at an earlier stage.
If you would like to have your pap smear done or just want to know more about HPV, speak to Dr.Gan Kam Ling, Obstetrician and Gynaecologist at Gleneagles Penang. You can book your appointment to see Dr Gan here.


Add a Comment